What is PAD?
Peripheral Artery Disease, or PAD, is a general term that refers to artery disease anywhere outside of your heart, including the arteries that supply blood to your legs, arms, brain, kidneys, and other organs. This section focuses on disease in the arteries of the legs, the most common kind of PAD. Click here for links to information on other types of peripheral artery disease.
PAD reduces blood flow to the legs (sometimes referred to as “poor circulation”), and may cause pain or damage to tissues. Because PAD can make walking difficult, it can interfere with many aspects of your life. Women with PAD often have trouble performing daily tasks at work or at home and are forced to avoid activites they enjoy. Because the process that causes PAD affects blood vessels throughout your body, women with PAD have an increased risk of developing heart disease and stroke. Women with PAD are 2 to 6 times more likely to die of heart disease than women without PAD.1 Without proper treatment, your symptoms may gradually get worse over time. In severe cases, PAD can lead to problems that require amputation of a toe, foot, or leg.
The good news is that healthy lifestyle changes, medication, and procedures to clear blocked arteries can relieve PAD symptoms, improve your quality of life, and lower your risk of heart attack and stroke. If you don’t have PAD, you can take steps to prevent it altogether.
What causes PAD?
The most common cause of PAD is hardening of the arteries ( atherosclerosis), the gradual buildup of fatty deposits (called plaque) on the walls of the arteries that slow or block blood flow. Plaque buildup also causes the artery walls to stiffen, making them unable to widen when the tissues need more blood, such as during exercise.
Atherosclerosis is the same process that causes coronary artery disease when it happens in the arteries that supply blood to the heart, and can cause a stroke when it blocks blood flow in the arteries that supply blood to the brain.
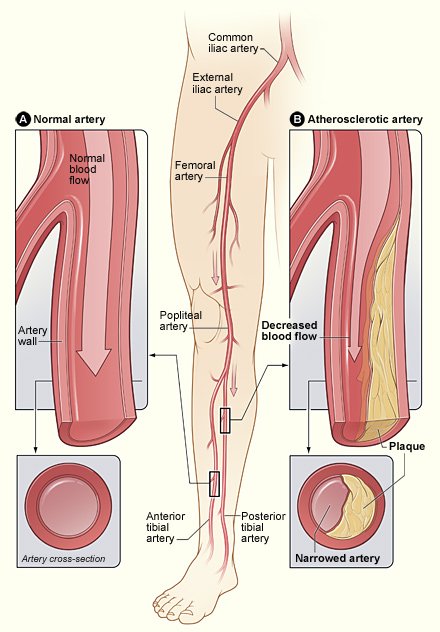
An illustration of how PAD impairs blood flow in the leg. PAD can occur anywhere in the leg arteries.
A: Blood flow through a normal leg artery. B: Blood flow through an artery of a person with PAD.
How common is PAD?
PAD affects more than 8 million Americans, including nearly 4 million women.2 This is 1 out of every 16 people aged 40 and older, and 1 in 5 people aged 70 or older.3 PAD is slightly more common in men than in women (1 in 5 older men versus 1 in 6 older women). One study had doctors screen their own patients with a questionnaire and a simple painless test called the ankle-brachial index. Nearly 1 in 3 women and men older than 70, or older than 50 who smoked or had diabetes, were found to have PAD!4
Despite how common PAD is and the serious risk of heart disease and stroke that goes along with it, awareness of PAD is low. In one survey of 2501 adults, only 1 in 4 were familiar with PAD. Among those who had heard of the disease, fewer than half were aware of the major risk factors, and only 25% knew that PAD increases your risk of heart attack and stroke.5 It is crucial to educate yourself about PAD so that you can recognize the symptoms and seek treatment before it causes serious problems.
What are the symptoms of PAD?
Because PAD develops gradually, in the early stages the disease may not cause any symptoms at all. As the disease progresses, most women will experience one or more of these common symptoms of PAD:
- Cramping, aching, numbness, tiredness, weakness, or burning in your buttock, thigh, calf or foot that occurs when walking and goes away when you rest. This pain is called intermittent claudication. It does not usually occur while sitting or standing still.
- Numbness in your legs or feet when you are at rest. Your skin may appear pale and feel cool to the touch.
- Foot or toe pain or tingling that does not go away with rest, and may disturb your sleep. The pain may be worse when the leg is elevated and improve when you hang your legs over the side of the bed.
- A feeling that the hip or leg is “giving out” during walking
- Skin wounds or ulcers on your legs or feet that heal slowly or do not heal at all
While claudication is considered the “classic” sign of PAD, most women and men with PAD do not have typical leg symptoms during exercise.2 In one study of 7715 elderly subjects (60% were women), only 5% of women and 9% of men with PAD reported claudication.6 About half of women with PAD have leg symptoms other than claudication. Many women do not experience leg pain at all, and the only way to tell that they have PAD is during a doctor’s examination.
Although many women do not think of leg pain or tiredness as a serious problem, pain in your legs is not a normal sign of aging. Proven treatments are available to relieve PAD symptoms and prevent complications, so be sure to discuss with your doctor any symptoms you experience.
See also: Symptoms of PAD
Who is at risk for PAD?
Your risk of PAD increases as you get older. Women 50 years or older have a higher risk of PAD than younger women, and women 70 or older are automatically considered at high risk for the disease. Your risk for PAD is also increased if you:
- Smoke or used to smoke
- Have diabetes
- Have high blood pressure
- Have high cholesterol
- Have a family history of artery disease (PAD, heart attack, or stroke)
- Have suffered a heart attack or stroke in the past
- Are African-American
- Have high levels of markers of inflammation in your blood, such as C-reactive protein and homocysteine
If these conditions sound familiar, it is because PAD shares many of the same risk factors with heart disease and stroke because they have a common cause (atherosclerosis). Diabetes and cigarette smoking have an especially powerful effect on your risk of developing PAD, with diabetes increasing your chances by up to 4 times and smoking by up to 6 times.6-8 Taking steps to prevent and control your risk factors for PAD will also reduce your risk of heart disease and stroke.
See Am I at Risk for PAD? (coming soon) to evaluate your risk.



